The 26 Review
- What is Plantar Fasciitis Inflammation of the plantar fascia, a thick ligament on the bottom of the foot attaching to the heel bone.
- Causes lack of arch support, fascial tear, gait abnormalities, improper shoes, obesity, soft tissue mass
- Symptoms sharp / stabbing pain (especially upon standing up in the morning) in the heel, pain in the arch of the foot
- Diagnosis physical examination, X-ray, Ultrasound, MRI
- Treatment rest, ice, anti-inflammatory medication, orthotics, lifestyle changes, injections, physical therapy, surgery
Heel Pain: Plantar Fasciitis E-Book

PLANTAR FASCIITIS
Embark on a journey to pain-free living with our exclusive ebook focused on a complete guide to plantar fasciitis. Unlock the secrets to soothing your feet and reclaiming your stride. This guide is your key to stepping confidently into a life without heel pain. Download now for the first step towards happy, healthy feet!
Let’s take a closer look…
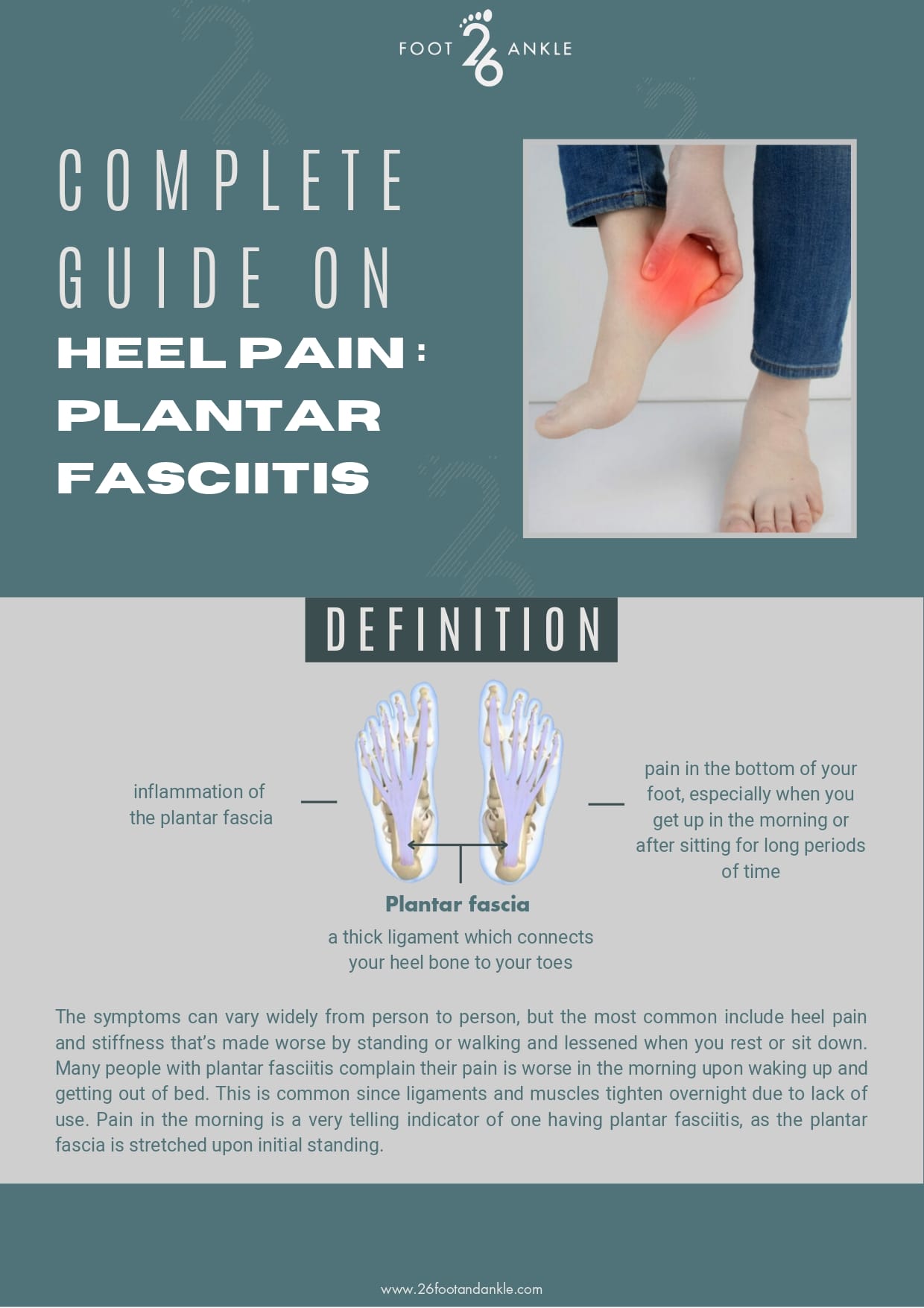
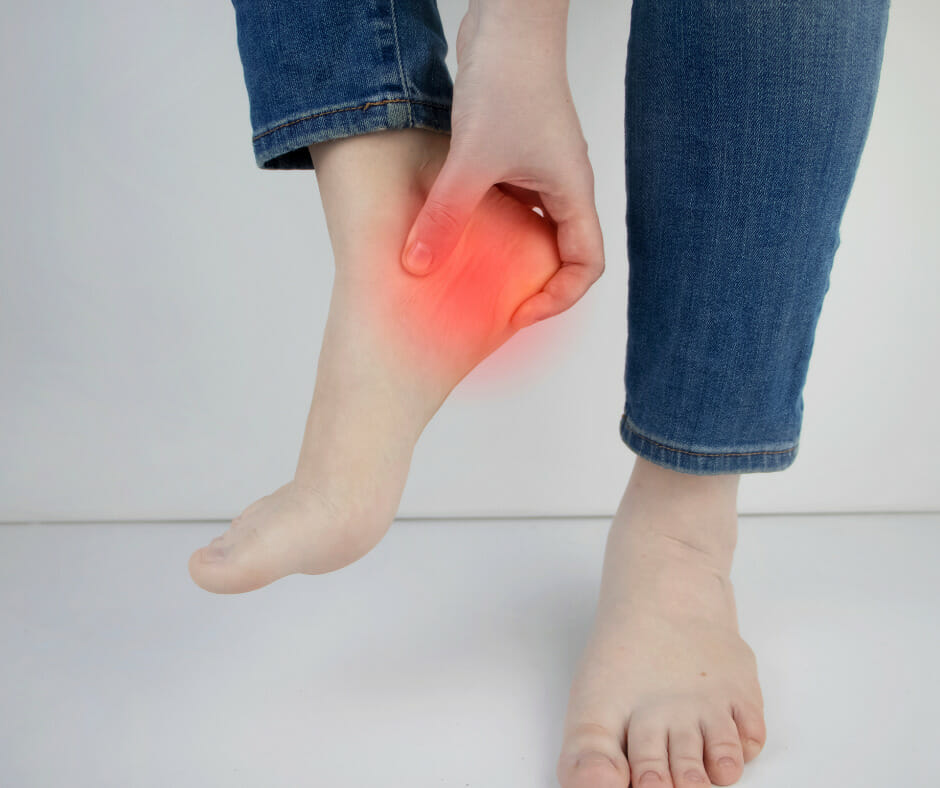
Plantar fasciitis is inflammation of the plantar fascia, a thick ligament which connects your heel bone to your toes. This presents as pain in the bottom of your foot, especially when you get up in the morning or after sitting for long periods of time. The symptoms can vary widely from person to person, but the most common include heel pain and stiffness that’s made worse by standing or walking and lessened when you rest or sit down. Many people with plantar fasciitis complain their pain is worse in the morning upon waking up and getting out of bed. This is common since ligaments and muscles tighten overnight due to lack of use. Pain in the morning is a very telling indicator of one having plantar fasciitis, as the plantar fascia is stretched upon initial standing.
Plantar fasciitis is one of the most common foot problems faced by individuals today, and with good reason: A growing number of people are putting on shoes that don’t properly support their feet and the activities they are engaged in. Spending long hours on their feet at work or school increases the risk of developing plantar fasciitis. Fortunately, plantar fasciitis can be treated through several different methods, some of which are more invasive than others but all of which are effective at reducing heel pain and improving your quality of life.
Causes
Plantar fasciitis is caused by repetitive stress to the plantar fascia, the ligament that runs along the bottom of your foot. This can be from activities such as running, dancing, or even standing for long periods of time. It can also be caused by ill-fitting footwear. The added stress on your feet causes the fascia to become inflamed and leads to heel pain over time. If not properly addressed and treated, heel spurs can form at the base of your heels which are bony protrusions the body creates to compensate for the inflammation and tension that is being caused. There are several risk factors that can increase your chances of developing plantar fasciitis: these include having flat feet or high arches, being overweight, wearing shoes with poor support, and having tight calf muscles.
Not all heel pain and arch pain is caused by inflammation of the plantar fascia where it attaches to the heal bone. In rare cases, a stress fracture or bone tumor can develop in the heal bone, leading to constant heel pain. Additionally, some individuals may be predisposed to hereditary conditions such as soft tissue masses that develop in the plantar fascia. These painful conditions can mimic plantar fasciitis but require a different treatment plan from typical heel pain and arch pain.
Symptoms
Plantar fasciitis pain usually increases over time and is felt most at the bottom of the foot close to one’s heel. Sometimes plantar fasciitis pain can be sudden and feel like a stabbing knife after you take a misstep. Something as simple as raising on the balls of your feet to grab something from a high cabinet can activate this sudden stabbing pain. Plantar fasciitis is often worse in the morning because the tissue and ligaments tighten up overnight. The pain usually improves with activity during the day; however, it can worsen with prolonged standing or walking. If you have plantar fasciitis, you may also notice swelling or redness and warmth in your heel area. Some individuals don’t experience pain at the base of their heel but more in the arch of the foot. This plantar fasciitis pain is also sharp in nature and is worse as the day progresses with walking.
Diagnosis
Your doctor will do a physical examination of your feet and ask about your medical history and any other factors that could be contributing to your experiencing or development of plantar fasciitis. This would include any recent injuries, health history, weight gain, recent stress level, and physical activity. Your doctor may also request that you bring in a pair or two of the shoes you wear the most throughout the week. While this may seem odd, a Podiatrist can examine the inside and outside of our insoles and can determine the way you distribute pressure while walking as well as what kind of arch support you are currently using. Your doctor may also order X-rays or an Ultrasound initialing to rule out other potential sources of the pain such as a stress fracture. In some cases, an MRI may be necessary to gather more information when individuals are experiencing persistent pain.
Treatment For Plantar Fasciitis
Most people with plantar fasciitis improve within 6-10 months of starting simple, nonsurgical treatments. Once diagnosed, your doctor will most likely prescribe a treatment plan that includes utilizing over-the-counter anti-inflammatories, daily foot and calf stretches several times a day (especially when you first get up in the morning) and wearing shoes that have good arch support and cushioning. Your doctor may also suggest avoiding high heels, flip-flops, or shoes with little support for a season, icing to reduce your inflammation, and possibly steroid injections. Additional treatments for plantar fasciitis include being fitted for custom orthotics, using a night splint when you sleep to keep your muscles stretched, and using a supportive foot ankle brace throughout the day. Once the severity of pain decreases after these initial treatments, it is important to always use supportive shoes and to replace all old and broken-down shoe gear.
Regenerative medicine options such as laser therapy, shock wave therapy, and platelet rich plasma (PRP) injections, are alternative options to consider opposed to surgery. In only the most severe cases is a surgery recommended for plantar fasciitis. This is typically after all non-surgical treatments have been utilized and exhausted with little to no improvement (which is rare) and if your plantar fasciitis is affecting your quality of life. Typical surgery for a severe case of plantar fasciitis involves releasing part of the plantar fascia ligament to alleviate the tension and swelling. Depending on the type of surgery, recovery can be between 2-6 weeks.