The 26 Review
- What is a Diabetic Foot Ulcer? A sore that develops in diabetics that heals slow and typically seen in the bottom of the foot
- Causes Poor circulation, high blood sugar, nerve damage, and skin irritation from wearing ill-fitting shoes
- Symptoms Slow healing wound with foul odor, drainage, swelling, and pain around the affected area.
- Diagnosis Physical examination, wound culture, blood tests, X-ray, MRI
- Treatment Antibiotics, topical medications, skin grafts, off-loading shoe or boot, daily wound care, surgery
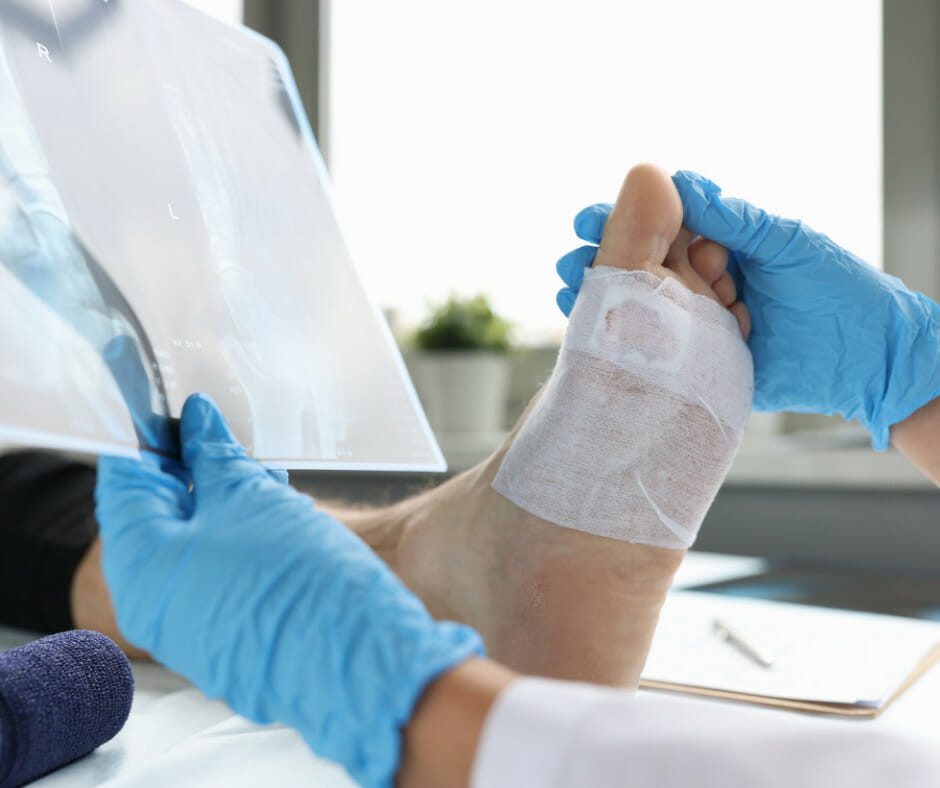
Let’s take a closer look…
Foot ulcers are a common form of skin wound. These wounds are a direct result of the skin tissue in the foot breaking down and revealing the layers of skin, muscle, and bone underneath. Most commonly, these ulcers are found on the balls of the feet and under the toes. Foot ulcers are typically a common complication that comes with Diabetes, especially if said illness is not being managed correctly. The majority of people won’t develop foot ulcers, however all people with diabetes are at a higher risk of developing such ailment. Failure to manage one’s diet, wear correct shoes, and properly manage one’s health including daily exercise routine and insulin treatment, will put people with Diabetes at a larger risk of developing foot ulcers. Treatment for diabetic foot ulcers may vary depending on the causes. Diabetic foot ulcers may show signs of early onset Peripheral Neuropathy. Continue reading more to learn about Diabetic Foot Ulcers, how to prevent them, and how to treat them.
Causes
Diabetic foot ulcers are an open sore or wound commonly located on the bottom of the foot. This ailment occurs in approximately 15 percent of patients with diabetes. People with Diabetes most commonly obtain ulcers caused by high blood sugar, poor circulation, nerve damage, and/or from wounded feet as a direct result from wearing improper or poor shoes. Having poor blood circulation does not allow for blood to flow to the feet efficiently, causing ulcers, as well as making it more difficult for ulcers to heal. Hyperglycemia or high blood sugar restrains the healing process of feet infected with an ulcer(s). Peripheral Neuropathy can affect the nerve endings in the feet long term. Long-term nerve damage can lead to loss of feeling in the feet, as well as tingly or painful experiences. Having nerve damage reduces the sensitivity in the feet, resulting in wounds or ulcers to exist without any trace. Combine these health issues with poor fitting shoes that cause abnormal rubbing and blisters on the feet will eventually develop a foot ulcer. A podiatric physician can physically examine and treat ulcers, in conjunction with testing the foot for neuropathy.
Symptoms
One of the key first signs to look out for when dealing with skin wounds, is whether the foot ulcer has been draining. Drainage with unusual swelling, irritation, redness and odors can also be an early indication of diabetic foot ulcers or infection. Eschar or black tissue will be the most visible sign of a serious foot ulcer, furthermore an infection within said foot ulcer. Black tissue appears due to the lack of healthy blood flow surrounding the area in which the ulcer resides. Other signs of an infected diabetic ulcer may appear as partial or complete gangrene. Gangrene refers to the tissue death around an infected area. In this case, you may come across foul odors, discharge, pain, and numbness. That being said, symptoms of a diabetic foot ulcer(s) are not always obvious, until it has become infected. Speak with your Podiatric physician if you begin to see any skin discoloration, irritation, calluses, or feel pain or numbness. If untreated, diabetic foot ulcers could cause abscesses (infection) and extend to other areas of the feet and legs.
Diagnosis
When diagnosing Diabetic Foot Ulcers, clinical physicians may use the Wagner Ulcer Classification System. This classification system enables doctors to determine the severity of the ulcer on a 0 to 5 scale.
• 0 → absence of open lesions; skin wound may have healed
• 1 → typical ulcer without penetration to layers deep underneath skin
• 2 → deeper ulcer that reaches either the tendon, bone or joint capsule
• 3 → deeper tissues can be located; accompanied with abscess, osteomyelitis or tendonitis
• 4 → small amounts of gangrene in a portion of the heel or ball of the foot
• 5 → extensive gangrene involving the entire foot
Depending on the state of the diabetic foot ulcer, a Podiatrist clinical experience is the best means of diagnosing and properly treating Diabetic Foot Ulcers. X-rays are obtained to determine if the underlying bone is involved. Prominent bones spurs or abnormalities in the bone such as positioning may be causing the wound to develop. In these cases, either the prominent bone can be removed or accommodated with a shoe modification. The X-rays can also be used to determine if the bone has become infected (Osteomyelitis). MRI is the gold standard for determining if the bone is involved if it is unclear on an X-ray. MRIs can become useful for evaluating the soft tissues for an additional infection. Wound cultures and sometimes blood tests are obtained in the setting of infected ulcer(s), as these tissue sample procedures are superior for diagnosing and treatment. Tissue samples such as a bone biopsy can provide more accurate results when identifying infectious pathogens.
Treatment For Diabetic Foot Ulcer
When a Diabetic Foot Ulcer is identified, beginning treatment almost immediately has proven to be incredibly important. The faster an ulcer is treated, the less likely infection can and will occur as well as preventing amputation. There are a few preventive measures that can be taken for people apart of the high-risk community. Some preventive measures include maintaining tight control of blood glucose levels, cleansing the wound daily, bandaging the wound, and not walking barefoot. Staying off your feet is one of the best ways to avoid pain and allow for the ulcer to heal. Off-loading the wound in a padded shoe or walking boot aids in distributing the pressure of walking, prohibiting the infection to worsen or spread. Patients may be asked to wear special footwear, a brace, specialized castings, and/or use a wheelchair or crutches. As mentioned before, bandages and dressings are appropriate for wound management, in addition to topical medications. In some cases, Podiatrists may initiate daily wound care to facilitated healing by way of wound debridement. Debridement is the removal of dead / damaged skin or tissue from a wound and typically done in the office setting. A sample of the tissue surrounding the diabetic foot ulcer may be sent to a lab to determine which antibiotic may help best. Minor procedures such as skin grafting can also help aid in quicker healing times. In serious cases when infections develop, your doctor may order additional X-rays or an MRI to aid in surgical planning as removal of additional tissue including bone may be required to prevent further infection or damage to the feet and legs.